Our next feature for National Athletic Training Month and Women’s History Month is a remarkable woman named Jessica Scott, DPT, ATC, CSCS, TSAC-F. She’s a force in athletic training and...

Introducing Dawn Gulick, PhD, PT, AT, CSCS– our first feature in HawkGrips’ “Women in Athletic Training” series for March, marking both National Athletic Training Month & Women’s History Month. Dawn’s...

IASTM stands for “Instrument Assisted Soft Tissue Mobilization”. This means, use of a tool or instrument to address and mobilize soft tissue structures.

We got to sit down with Scott Dolly, MS, ATC, CSCS, and Owner/CEO of Evolution Human Performance and Rehabilitation in Winchester, VA. A top sports performance and rehabilitation specialist, Scott...
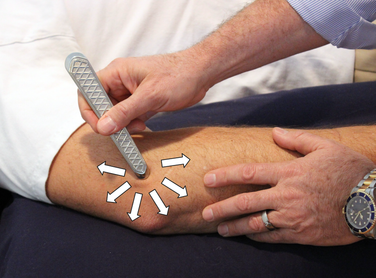
What is Tennis Elbow? Lateral Epicondylitis, or Tennis Elbow, occurs on the outside of the elbow and sometimes in the forearm and wrist. Pain is the primary symptom. It is...
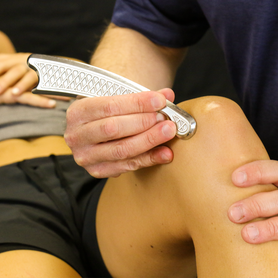
Runner’s knee or patellofemoral pain syndrome (PFPS) is common not only in serious runners but in many walks of life. The condition shows up as dull pain around the front...